Let’s address some of the most common questions asked about gastroparesis (GP).
What is gastroparesis?
Gastroparesis is a condition where symptoms occur and the stomach empties too slowly. No blockage is evident. The delayed emptying is confirmed by a test.
How common is gastroparesis?
While the incidence and prevalence of gastroparesis are not well-defined, it is estimated to affect up to 5 million individuals in the United States.[1] Gastroparesis isn’t common. Out of 100,000 people, about 10 men and about 40 women have gastroparesis. It is also important to note that symptoms that can be similar to gastroparesis can occur in about 1 out of every 4 adults in the United States.
Who is more likely to get gastroparesis?
- People who have diabetes.
- Have had surgery on your esophagus, stomach, or small intestine which may injure the vagus nerve.
- People who have had certain cancer treatments, such as radiation therapy on your chest or stomach area.
What are the signs and symptoms of gastroparesis?
Symptoms usually occur during and after eating a meal. Typical symptoms include:
-
-
- Nausea and/or vomiting
- Retching (dry heaves)
- Stomach fullness after a normal sized meal
- Early fullness (satiety) – unable to finish a meal
- Stomach pain and discomfort
-
There may also be bloating, heartburn, and stomach discomfort or pain. Decreased appetite may result in weight loss.
Learn More about Signs & Symptoms
What causes gastroparesis?
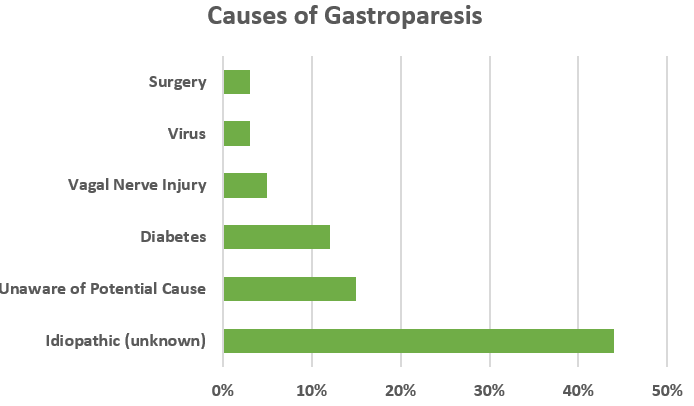
Most often in people with gastroparesis, the cause is unknown and is termed “idiopathic.” Symptoms may begin following a virus infection. Other possible causes include diabetes, surgeries, some medications, and other illnesses.
How do I know if I have gastroparesis?
Diagnosis is by a doctor who will perform a physical exam and some tests. Tell your doctor about any medications you are taking. If the doctor suspects gastroparesis, a test to measure how fast the stomach empties is needed to confirm the diagnosis.
Learn More about Diagnosis & Tests
How is gastroparesis treated?
Treatments are aimed at managing symptoms long term. This involves one or a combination of dietary and lifestyle measures, medications, and/or procedures that may include surgery.
Mild symptoms that come and go may be managed with dietary and lifestyle measures. Moderate to more severe symptoms additionally may be treated with medicines to stimulate stomach emptying and/or reduce nausea and vomiting.
Severe symptoms that are harder to treat may require added procedures to maintain nutrition and/or reduce symptoms.
What Are Some Dietary and Lifestyle Measures?
Changing eating habits can help control gastroparesis and make sure you are getting the right amount of nutrients, calories, and liquids. A dietitian can help design a dietary plan to meet your needs and help treat the disorder’s two main complications: malnutrition and dehydration.
Gentle physical activity is also recommended after each meal. Taking a walk or doing yoga can help stimulate digestion.
If you have diabetes, blood glucose levels will need to be controlled as well as possible. Blood glucose levels go up after stomach contents empty into the small intestine, and this is irregular in gastroparesis.
Learn more about gastroparesis dietary and lifestyle measures.
What Medications Can Help?
Prokinetic (promotility) agents help the stomach empty more quickly and may improve nausea, vomiting, and bloating. Antiemetic agents are used to treat nausea and vomiting.
What Types of Procedures Can Be Done?
Severe symptoms sometimes result in dehydration, loss of essential minerals (electrolyte imbalances), and malnutrition requiring hospitalizations. Special treatment measures to help manage may include:
-
-
- enteral nutrition,
- parenteral nutrition,
- gastric electrical stimulation, or
- other surgical procedures.
-
Learn More about Procedures & Surgery
Be sure to ask questions so you understand any treatment and options, know the risks as well as benefits, and know what to do if side effects occur or symptoms return.
Keep hydrated and as nutritionally fit as possible. Persistence pays off, as most people with gastroparesis ultimately will do well.
Do you have more questions that weren’t addressed here? Feel free to reach out to IFFGD to request more information or submit your questions.
Updated October 2023
Reference
Adapted from IFFGD Publication: 551-Gastroparesis
NIH, National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), Gastroparesis Clinical Research Consortium. www.niddkrepository.org/studies/gpcrc (Accessed January 16, 2018)
